
For all the numerous risk factors that can lead to the development of substance abuse, the fundamental dynamic of gender has a huge role to play. Whether male, female, or transgender, drug abuse and gender are closely intertwined, which makes a significant difference in how people of respective genders are at risk for addiction, as well as how they are treated.
Does Gender Matter?
 Substance abuse is a very complicated issue, and so is gender; put the two together, and more questions are raised. “Why do men take more drugs than women?” asks The Telegraph, while Psychiatric Times puts it another way: “Substance abuse in women: does gender matter?”[1], [2] It absolutely matters, according to the review in Psychiatric Times. As a sign of how seriously scientists and researchers are asking the question, 90 percent of scientific and medical literature on the topic of abuse and gender had been published in the 15 years between 1990 and 2005.
Substance abuse is a very complicated issue, and so is gender; put the two together, and more questions are raised. “Why do men take more drugs than women?” asks The Telegraph, while Psychiatric Times puts it another way: “Substance abuse in women: does gender matter?”[1], [2] It absolutely matters, according to the review in Psychiatric Times. As a sign of how seriously scientists and researchers are asking the question, 90 percent of scientific and medical literature on the topic of abuse and gender had been published in the 15 years between 1990 and 2005.
A big reason for this new focus is that the gender gap has been declining for the past few decades, prompting speculation that women are on the cusp of earning (or even surpassing) their male colleagues.[3] With this extra spending money comes an increase in social status, which results in “American women […] drinking more like men,” says Newser.[4] This article mentions a 2015 report from the National Institutes of Health, entitled “Male and Female Drinking Patterns Becoming More Alike.”[5] In the mid-2010s, women have more earning power, more access to alcohol, and more advertising and marketing that is catered to the female experience of drinking, even when it comes down to suggesting the kinds of drinks that women should have. According to Attn, “beverage-based gender stereotypes have become an observable norm.”[6]
Bound by Biology
This upward mobility has empowered many women to step out of the shadow of traditional gender roles which bound previous generations, but it also exposes these women to health risks and dangers. Some of those risks are tied to biology; a woman has to consume less alcohol than a man in order for intoxication to take place. This is because women have less total body water than men, writes the Psychiatric Clinics of North America journal, so women achieve greater concentrations of blood alcohol, even if they consume the same amount of alcohol itself.[7] Additionally, women lack an enzyme (gastric alcohol dehydrogenase) that helps them metabolize alcohol as quickly as men, who do not lack the enzyme. One of the researchers who published this finding in the Alcoholism: Clinical and Experimental Research journal commented that the deficiency contributes to the female gender being “more susceptible to toxic amounts of alcohol” than the male counterpart.[8] Similarly, an imaging procedure that creates detailed scans of the human body has shown that it takes less alcohol to affect a woman’s brain than it takes to affect a man’s, according to another study published in the same journal.[9]
Other imaging operations show that the effects are not limited to alcohol. Among people who take cocaine, says Biological Psychiatry, the female brain responds much more actively to the drug than the male brain does.[10]
All the signs point to women being more vulnerable to the consequences of drinking, says the review from Psychiatric Times, which notes that the negative effects are primarily psychological and physiological.

Men and Gender Roles
Women may be at greater risk of suffering the risks of alcohol and drug use, but the question posed by The Telegraph – “Why do men take more drugs than women?” – still lingers. According to statistics published by the British government, men are thrice as likely to regularly consume illegal drugs (everything from marijuana to cocaine) than women.
Even though young women drink as much as men, it is men who consistently use drugs more than women. Men, says The Telegraph, are less likely to think about the risks of their drug behavior than women.
One government survey found that 27 percent of men had no concerns for their health when it came to smoking cannabis, while only 15 percent of women thought it would be safe to do so. Just 1 percent of women believed it was safe to take cocaine; but among men, that number rose to 5 percent.
Dr. Adam Winstock, a psychiatrist who specializes in drug abuse and addiction, says that men are “more naturally prone to take risks,” which includes the risk of taking dangerous drugs. Men tend to have unhealthier lifestyles than women, to die younger, and to have “less insight into [their] health and wellbeing.” Genetically and evolutionarily, men are “generally predisposed to engage in a whole bunch of risky behaviors,” partly due to gender roles.[11]
Masculine Gender Role Stress
 Gender roles are a massive construct in male and female behavior, and this is significantly represented in how either gender responds to substance abuse. In 1998, the Journal of Gender, Culture and Health looked at masculine gender role stress, which develops in men “who are highly committed to the male role.” This involves constant displays of strength (physical, emotional, and otherwise) and hyperavoidance of weakness or femininity. Men who struggled with pressure to display high levels of masculine gender roles were found to have “more severe alcohol [and drug] dependence” than men who had little to no stress related to their perceived gender role. Researchers also discovered that men who displayed masculine gender role stress were more likely to abuse drugs and alcohol as a response to emotions they considered negative, as well as physical discomfort, and to believe that they were in control of their substance abuse.[12]
Gender roles are a massive construct in male and female behavior, and this is significantly represented in how either gender responds to substance abuse. In 1998, the Journal of Gender, Culture and Health looked at masculine gender role stress, which develops in men “who are highly committed to the male role.” This involves constant displays of strength (physical, emotional, and otherwise) and hyperavoidance of weakness or femininity. Men who struggled with pressure to display high levels of masculine gender roles were found to have “more severe alcohol [and drug] dependence” than men who had little to no stress related to their perceived gender role. Researchers also discovered that men who displayed masculine gender role stress were more likely to abuse drugs and alcohol as a response to emotions they considered negative, as well as physical discomfort, and to believe that they were in control of their substance abuse.[12]
For men who take drugs or alcohol, the action of doing so reinforces their image of themselves as men, according to the Archives of General Psychiatry.[13] Even the experiences of different substance consumption speak to the distinctiveness of each gender. Men tend to smoke to reduce tension and improve mood; women tend to smoke to bond in social settings. Smoking is an “instant conversation starter” and creates an “immediate bond with strangers,” says the Journal of American College Health.[14] For women, smoking accounted for a “predominant influence” in different social contexts: spending time with other smokers, attracting potential romantic/sexual partners, drinking alcohol, and frequenting places where alcohol is available.[15]
Call Now (619) 577-4483
Men, Women, and Drug Use
Gender roles also limit women, even as women (as a demographic) have more spending and cultural power than they did a generation ago. Dr. Winstock tells The Telegraph that there still exists a great deal of stigma around women who take drugs, while male drug abusers receive no such shame. Women who do consume drugs are less likely to tell their friends and family about it, which has the effect of limiting access to more drugs (but also limiting access to help and treatment). But having a male partner who uses drugs is a significant risk factor for whether the female partner in the relationship will pick up the habit; living with a partner with a substance abuse problem presents serious sources of stress and threats to wellbeing, notes the American Journal of Drug and Alcohol Abuse. This can contribute to the development of an addiction with the female partner, and it can also stymie recovery and rehabilitation since the home environment is not conducive to sobriety.[16]
While women in relationships tend to pick up substance abuse through their partner, men, on the other hand, are more likely to start drug use with their peers, which can then develop into a substance abuse problem.
On college campuses, where drug use is widespread in an era of greater acceptance of the use of mind-altering chemicals, almost 40 percent of males reported smoking marijuana, while only 30 percent of women admitted to the same.[17] As a further sign of the risk-taking behavior of men, the Journal of Adolescent Health found that male students who drank alcohol also tended to abuse prescription drugs (such as Adderall, for staying up later and boosting mental acuity); researchers found no such connection existed among female students. Similarly, male students who had previously used drugs had “an increased likelihood of substance abuse of prescription [painkillers] during young adulthood”; but among female students, only previous marijuana use offered any connection to substance abuse.[18]
Menstruation and Drug Abuse
 One of the most striking differences between the genders, and one that makes a notable impact in how men and women respond to substance abuse differently, is that of menstruation. Functional magnetic resonance imaging has shown how estrogen and progesterone hormones are not only responsible for ovulation and reproduction, but also how they also impact “a large number of cognitive and affective functions,” says Science Daily. Some of those functions include the regulation of the reward system in the brain, which is how menstruation and substance abuse overlap.[19]
One of the most striking differences between the genders, and one that makes a notable impact in how men and women respond to substance abuse differently, is that of menstruation. Functional magnetic resonance imaging has shown how estrogen and progesterone hormones are not only responsible for ovulation and reproduction, but also how they also impact “a large number of cognitive and affective functions,” says Science Daily. Some of those functions include the regulation of the reward system in the brain, which is how menstruation and substance abuse overlap.[19]
Brain scans show that the regions of the brain that process pleasure, rewards, and the anticipation of receiving more pleasure and reward become significantly more activated during menstruation, when estrogen levels are significantly higher.[20] This may be why women respond to cocaine to a much greater degree than male users of the drug, and why women tend to use cocaine to a “more severe” degree than male users.[21]
Female drug users have reported that where they are in their menstrual cycle has an impact on their drug use. Women who use cocaine during their luteal phase (which begins after ovulation) do not experience as strong a high as when they take cocaine during their follicular phase (which ends with ovulation).
The effect is such that even women who are trying to quit cocaine might be more susceptible to relapse during the follicular phase of their cycle, writes Experimental and Clinical Psychopharmacology, simply because they slipped up at the wrong time in their cycle.[22]
Further in the study of how gender-specific hormones might affect substance abuse, Trends in Pharmacological Sciences suggests that women tend to be more aware of the pleasurable sensations of drug consumption, primarily because estrogen activates receptors in the brain that increase the effects of the substances in terms of how quickly and powerfully they are felt.[23]
Unique Vulnerabilities
In fact, the overall temptation of taking dangerous and unhealthy substances “ebbs and flows with a woman’s monthly cycle,” says Scientific American. This means that women could be “uniquely vulnerable” to drug abuse and its effects, because of how powerfully female sex hormones (like estrogen and progesterone) affect the regions of the brain that regulate reward anticipation, and the response to substances that stimulate those regions.[24]
Female hormones don’t affect just the brain systems that control pleasure and rewards. They can make a mess of mental health, says Vice magazine. The Archives of Psychiatric Nursing writes of the “associations between psychiatric disorders and menstrual cycle characteristics.”[25], [26] On their own, women can experience any number of effects as part of a normal menstrual cycle, such as mood swings, depression, anxiety, reduced cognitive ability, and sleep disorders. A cycle could exacerbate a pre-existing mental health condition in a woman, which might also contribute to the development (or further exacerbation) of substance abuse. Women are twice as likely as men to suffer from major depression (and twice as likely as men to develop clinical anxiety), but this goes misdiagnosed as much as 50 percent of the time.[27] The American Psychological Association explains that 70 percent of the prescriptions for antidepressants are written for female patients, “often with improper diagnosis and monitoring,” leading to situations where women became addicted to their prescription drugs.[28]
Hormones, Mental Health, and Drug Addiction
Suffering traumatic events can be a direct cause of depression and anxiety, but women are twice as likely to develop post-traumatic stress disorder than men. This is because women have an increased fear response to a traumatic event, due to what the Journal of Psychiatric Research called an “acquisition of conditioned fear.”[29] Again, hormones may play a role in this; research out of Harvard and Emory University suggest that some women’s vulnerability to anxiety disorders may be a result of low estrogen levels, which make women more susceptible to suffering greater degrees of trauma if a distressing event takes place at certain points during their menstrual cycles. High levels of estrogen can offer some measure of protection from emotional upheaval. Researchers theorized that women are most at risk for developing PTSD during periods of low estrogen during their menstrual cycle, which they may seek to self-medicate with the use of drugs and alcohol – the effects of which are magnified by the range of psychological and neurochemical changes brought about by menstruation.[30]
- Treatment and the Male Gender
-
In the same way that gender roles account for a significant risk factor in determining the likelihood of abuse, they can also influence barriers to and methods of treatment. Men tend to be more reluctant to admit that their drinking or drug use has gotten out of control, and they are thus less likely to seek out help by themselves. The American Psychological Association writes that it usually takes a crisis (a family intervention, a DUI, or a court order) for a man to acknowledge his drug abuse and get treatment for it.[31] The American Journal of Drug and Alcohol Abuse further writes that men usually have better treatment outcomes if there are ultimatums associated with their treatment; that is, facing prison time, divorce, or job loss works well in motivating men to see their treatment through.[32]
There persists an idea that “real men don’t whine about their physical, mental, or emotional problems,” but as Psych Central warns, a failure to address psychological and behavioral issues can lead to clinical depression.[33]
For men, a literature review by Westminster College found that male clients responded better to inpatient programs, which are traditionally very structured and organized. Men reported lower rates of relapsing after graduating from such programs; on the other hand, men in outpatient programs, which grant a greater degree of personal freedom, did not fare as well as women. Men who participate in group activities and group therapy relapsed less, likely because sharing their experiences with other men (who made the same mistakes) cultivated a sense of solidarity and community, which treatment programs look to emphasize as part of their rehabilitation paradigm.[34]
Some treatment centers try to use traditional concepts of masculinity to help their male clients overcome the challenges that led to the substance abuse. Adventure therapy, which is primarily outdoors in nature (e.g., camping, hiking, fishing, etc.) encourages men to work together. In this environment, asking for help, trusting others, and honestly admitting weaknesses are the only ways to get things done, and the lessons learned are applied to everyday situations that will help sobriety in the real world.[35]
- Treatment and the Female Gender
-
When it comes to women, the female gender is often better at distinguishing emotions and then actively doing something to address the problems at hand.[36] However, gender norms can also work against women; the pressure to maintain family duties and obligations, to the point of curtailing treatment by inducing feelings of guilt for being away from children and household work, compels many women to leave treatment early (compared to men who are likelier to remain in treatment for longer once they start). The Journal of Substance Abuse Treatment describes these as “severe problems” that result in women having generally lower treatment completion rates than men.[37]
As a way of working around this problem, some treatment facilities offer childcare as part of their services, allowing recovering mothers to be near their children during counseling and ensuring that the children are given appropriate attention and care when the mother is unavailable. Such services also remove children from environments that threaten their wellbeing – for example, a home environment where there is abuse or easy access to drugs and alcohol. The Gazette writes of a treatment center in Iowa that provides long-term residential services to women and children, as a response to there being a large number of mothers who dropped out of standard residential programs because they did not want to put their children in the state’s foster care program.[38]
Similarly, a facility in Rochester, New Hampshire, offers treatment specifically for pregnant and nursing women. The co-founder of the program told New Hampshire Public Radio that clients will receive group therapy, as well as parenting classes, in a home-like setting that emphasizes nurturing and support.[39]
Call Now (619) 577-4483
Drug Abuse and Transgender People
Understanding how men and women respond to substance abuse and treatment has shaped the entire addiction treatment industry. However, a greater (and more recent) focus on issues surrounding transgender and non-binary individuals, whose gender identity does not fit into categories of male and/or female, highlights how the scope of human sexuality and identity is evolving and, with it, how our grasp of addiction science and psychology is also changing.
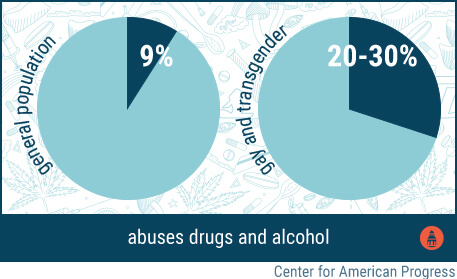
The Center for American Progress explains that while only approximately 9 percent of the general population abuse drugs and alcohol, the figure rises to 20 percent or 30 percent for gay and transgender people.[40] Specifically, men who engage in sexual activity with other men use marijuana 35 times more than men who engage in sexual activity with women; such men are also 12.2 times more likely to use methamphetamines and 9.5 times more likely to use heroin than their heterosexual counterparts.[41]
LGBT Discrimination and Temptation
 The high rates of substance abuse are largely due to LGBT individuals being subject to more frequent and severe forms of sex- and gender-based discrimination than cisgender individuals, resulting in major mental health disorders that compel drug abuse. Compounding the problem is that there is still widespread cultural ignorance of the nature of transgender identity (Live Science noted that the “T” in “LGBT” remains a source of confusion and misunderstanding.) and how best to treat transgendered people who are suffering from addiction.[42] To that point, only 6 percent of substance abuse centers in America (777 out of a total of 13,688) offered specialized programs for LGBT clients, according to a 2010 report from the Substance Abuse and Mental Health Services Administration.[43]
The high rates of substance abuse are largely due to LGBT individuals being subject to more frequent and severe forms of sex- and gender-based discrimination than cisgender individuals, resulting in major mental health disorders that compel drug abuse. Compounding the problem is that there is still widespread cultural ignorance of the nature of transgender identity (Live Science noted that the “T” in “LGBT” remains a source of confusion and misunderstanding.) and how best to treat transgendered people who are suffering from addiction.[42] To that point, only 6 percent of substance abuse centers in America (777 out of a total of 13,688) offered specialized programs for LGBT clients, according to a 2010 report from the Substance Abuse and Mental Health Services Administration.[43]
However, there is a strong cultural push toward alcohol and substance abuse from within LGBT communities. Tobacco and alcohol companies market directly to transgendered people through advertisements, using concepts of liberation and individualism to tap into the philosophies that empower many LGBT people to come out while also exploiting vulnerabilities and insecurities by making drugs and alcohol seem like an integral part of life as a transgendered person.[44]
This has had the effect of normalizing drug consumption across LGBT communities, which in conjunction with issues of social stress, harassment, and prejudice typically experienced by members of those communities (sometimes on an everyday basis), dramatically increases rates of addiction among transgendered people.[45]
Citations
[1] “Why Do Men Take More Drugs Than Women?” (July 2014). The Telegraph. Accessed December 5, 2016.
[2] “Substance Abuse in Women: Does Gender Matter?” (December 2006). Psychiatric Times. Accessed December 5, 2016.
[3] “Women’s Gains or Men’s Losses? A Closer Look at the Shrinking Gender Gap in Earnings.” (September 1995). American Journal of Sociology. Accessed December 5, 2016.
[4] “American Women Are Drinking More Like Men.” (November 2015). Newser. Accessed December 5, 2016.
[5] “Male and Female Drinking Patterns Becoming More Alike in the US.” (November 2015). National Institutes of Health. Accessed December 5, 2015.
[6] “How Alcohol Ads Influence What Women Are Expected to Drink.” (September 2015). Attn. Accessed December 5, 2016.
[7] “Gender Differences in Substance Abuse Disorders.” (June 1999). The Psychiatric Clinics of North America. Accessed December 5, 2016.
[8] “Enzyme Lack Lowers Women’s Alcohol Tolerance.” (April 2001). Scientific American. Accessed December 5, 2016.
[9] “Neuroimaging of Gender Differences in Alcohol Dependence: Are Women More Vulnerable?” (May 2005). Alcoholism: Clinical and Experimental Research. Accessed December 5, 2016.
[10] “Sex Differences in Brain Activation During Stress Imagery in Abstinent Cocaine Users: A Functional Magnetic Resonance Imaging Study.” (March 2005). Biological Psychiatry. Accessed December 5, 2016.
[11] “What Drives Men to Take Bigger Risks?” (September 2015). Bloomberg. Accessed December 6, 2016.
[12] “Masculine Gender Role Stress and Substance Abuse Among Substance Dependent Males.” (September 1998). Journal of Gender, Culture and Health. Accessed December 6, 2016.
[13] “Sex Differences in Availability Of β2*-nicotinic Acetylcholine Receptors in Recently Abstinent Tobacco Smokers.” (April 2012). Archives of General Psychiatry. Accessed December 6, 2016.
[14] “Characteristics of Social Smoking Among College Students.” (November-December 2006). Journal of American College Health. Accessed December 6, 2016.
[15] “From Partying to Parenthood: Young Women’s Perceptions of Cigarette Smoking Across Life Transitions.” (April 2006). Health Education Research. Accessed December 6, 2016.
[16] “Course, Severity, and Treatment of Substance Abuse Among Women Versus Men.” (November 2000). American Journal of Drug and Alcohol Abuse. Accessed December 6, 2016.
[17] “Race/Ethnicity and Gender Differences in Drug Use and Abuse Among College Students.” (2007). Journal of Ethnicity in Substance Abuse. Accessed December 6, 2016.
[18] “Previous Use of Alcohol, Cigarettes, and Marijuana and Subsequent Abuse of Prescription Opioids in Young Adults.” (February 2013). Journal of Adolescent Health. Accessed December 6, 2016.
[19] “Influence of the Menstrual Cycle on the Female Brain.” (February 2007). Science Daily. Accessed December 6, 2016.
[20] “Biological Basis of Sex Differences in Drug Abuse: Preclinical and Clinical Studies.” (November 2002). Psychopharmacology. Accessed December 6, 2016.
[21] “Comparing Levels of Cocaine Cue Reactivity in Male and Female Outpatients.” (February 1999). Drug & Alcohol Dependence. Accessed December 6, 2016.
[22] “Sex and Menstrual Cycle Differences in the Subjective Effects from Smoked Cocaine in Humans.” (August 1999). Experimental and Clinical Psychopharmacology. Accessed December 6, 2016.
[23] “Sex and Estrogen Influence Drug Abuse.” (May 2004). Trends in Pharmacological Sciences. Accessed December 6, 2016.
[24] “She’s Hooked: Allure of Vices Tied to a Woman’s Monthly Cycle.” (May 2010). Scientific American. Accessed December 6, 2016.
[25] “Associations between Psychiatric Disorders and Menstrual Cycle Characteristics.” (October 2009). Archives of Psychiatric Nursing. Accessed December 6, 2016.
[26] “Female Hormones Can Make a Bloody Mess of Your Mental Health.” (May 2015). Vice. Accessed December 6, 2016.
[27] “Anxiety Disorders in Women.” (2005). Anxiety Disorders Association of America. Accessed December 6, 2016.
[28] “Women and Depression.” (n.d.) American Psychological Association. Accessed December 6, 2016.
[29] “Sex Differences in Fear Conditioning in Posttraumatic Stress Disorder.” (January 2013). Journal of Psychiatric Research. Accessed December 6, 2016.
[30] “Estrogen and Female Anxiety.” (August 2012). Harvard Gazette. Accessed December 6, 2016.
[31] “Helping Men to Help Themselves.” (June 2005). American Psychological Association. Accessed December 7, 2016.
[32] “Gender Differences in Drug Treatment Careers Among Clients in the National Drug Abuse Treatment Outcome Study.” (August 1999). American Journal of Drug and Alcohol Abuse. Accessed December 7, 2016.
[33] “Real Men Don’t Get Help.” (May 2016). Psych Central. Accessed December 7, 2016.
[34] “Gender Differences in Substance Abuse Create a Need for Single-Gender Treatment Programs.” (n.d.). The Myriad. Accessed December 7, 2016.
[35] “The Relationship Between Masculinity Norms and Adventure Therapy Outcomes for Young Adult Men.” (n.d.) University of Texas Libraries. Accessed December 6, 2016.
[36] “Women Outperform Men When Identifying Emotions.” (October 2009). Science Daily. Accessed December 7, 2016.
[37] “Gender Differences in Problem Severity at Assessment and Treatment Retention.” (January 2001). Journal of Substance Abuse Treatment. Accessed December 7, 2016.
[38] “Heroin’s Hold: Heart of Iowa Offers Long-term Rehabilitation for Women and Children.” (June 2016). The Gazette. Accessed December 7, 2016.
[39] “In Rochester, Drug Treatment Program for Pregnant Women Opens with Wait List.” (December 2016). New Hampshire Public Radio. Accessed December 8, 2016.
[40] “Why the Gay and Transgender Population Experiences Higher Rates of Substance Use.” (March 2012). Center for American Progress. Accessed December 6, 2016.
[41] “Roughly 25 Percent of the LGBT Population Abuses Substances.” (March 2012). Out. Accessed December 7, 2016.
[42] “What is Transgender?” (November 2013). Live Science. Accessed December 6, 2016.
[43] “New National Study Shows That Only Six Percent of Substance Abuse Treatment Facilities Offer Specialized Services for Gays and Lesbians.” (June 2010). Substance Abuse and Mental Health Services Administration. Accessed December 7, 2016.
[44] “Tobacco and the GLBT Community.” (n.d.) American Cancer Society. Accessed December 7, 2016.
[45] “Prejudice, Social Stress, and Mental Health in Lesbian, Gay, and Bisexual Populations: Conceptual Issues and Research Evidence.” (November 2007). Psychological Bulletin. Accessed December 7, 2016.
